Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Genital Herpes
Condition Basics
What is genital herpes?
Genital herpes is one of the most common sexually transmitted infections (STIs). Most people never have symptoms, or the symptoms are so mild that people don't know that they're infected. But in some people, the infection causes occasional outbreaks of itchy and painful sores in the genital area.
What causes it?
Genital herpes is caused by a virus—either the herpes simplex virus type 1 or the herpes simplex virus type 2. You get infected when the virus enters your body. It can enter through a break in the skin or through moist areas such as the mouth, anus, and vagina.
What are the symptoms?
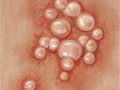
Most people never have any symptoms of genital herpes. But some people have painful or bothersome symptoms, such as itchy, painful blisters on the penis or around the vagina. The blisters break open and turn into oozing, shallow sores. Some people have flu-like symptoms, such as a fever and muscle aches.
How is it diagnosed?
Your doctor may diagnose genital herpes by examining you. He or she may ask you questions about your symptoms and how you think you were exposed to herpes. If this is your first outbreak, your doctor may take a sample of fluid from the sore for testing. You may also have a blood test.
How is genital herpes treated?
Although there is no cure for genital herpes, medicine can help. It can be taken during an outbreak to relieve pain and itching and help sores heal faster. It can also be taken daily to help prevent outbreaks. Home treatment, such as taking warm sitz baths, can help relieve discomfort from sores.
How can you prevent sexually transmitted infections (STIs)?
Here are some ways to help prevent STIs.
- Limit your sex partners. Sex with one partner who has sex only with you can reduce your risk of getting an STI.
- Talk with your partner or partners about STIs before you have sex. Find out if they are at risk for an STI. Remember that it's possible to have an STI and not know it.
- Wait to have sex with new partners until you've each been tested.
- Don't have sex if you have symptoms of an infection or if you are being treated for an STI.
- Use a condom every time you have sex. Condoms are the only form of birth control that also helps prevent STIs.
- If you had sex without a condom, ask your doctor if taking a preventive medicine is recommended. It may help prevent certain STIs if it's taken within 24 to 72 hours after unprotected sex.
- Don't share sex toys. But if you do share them, use a condom and clean the sex toys between each use.
Vaccines are available for some STIs, such as HPV. Ask your doctor for more information.
Cause
Genital herpes is caused by a virus—either the herpes simplex virus type 1 or the herpes simplex virus type 2. Either virus can cause sores on the lips and on the genitals. Type 1 more often causes cold sores. Type 2 more often causes genital sores.
You get infected when the virus enters your body. It can enter through a break in the skin or through moist areas such as the mouth, anus, and vagina.
Learn more
Symptoms
Symptoms of genital herpes can vary greatly from person to person. Most people never have symptoms. Sometimes the symptoms are so mild that you may not notice them. But some people have painful and bothersome symptoms. Symptoms may include:
- Outbreaks of itchy and painful blisters on the penis or around the opening of the vagina. The blisters break open and turn into oozing, shallow sores that take up to 3 weeks to heal.
- Flu-like symptoms, such as fever, headache, and muscle aches. You may also notice an abnormal discharge and pain when you urinate.
If you notice your first infection, the symptoms will generally appear about 2 to 14 days after you were exposed to genital herpes.
Symptoms of later outbreaks are usually limited to blisters, sores, and swollen lymph nodes. As time goes on, the outbreaks happen less often, heal faster, and don't hurt as much.
What Happens
When genital herpes symptoms appear, it's usually 2 to 14 days after a person is exposed to the virus. Sometimes people get their first symptoms months or even years after they're infected.
The herpes virus stays in your body for the rest of your life. After the first outbreak, it becomes inactive. Then, in most people, it gets active again from time to time and causes blisters and sores. Stress, illness, or menstruation may trigger a new outbreak.
Genital herpes can cause other problems—some serious—if the virus travels to other parts of the body. But this is rare.
If someone who's pregnant has a genital herpes blister or sore at the time of labor and birth, a cesarean (C-section) is usually done. In rare cases, a newborn can be infected with the herpes virus during birth. This can cause the newborn to have serious health problems that affect many body systems.
Learn more
When to Call a Doctor
If you haven't been diagnosed with genital herpes, call your doctor if you have:
- Painful blisters or sores in the genital or pelvic area.
- Burning or pain while urinating, or you can't urinate.
- Abnormal discharge from the vagina or penis.
- Reason to think you've been exposed to genital herpes.
If you have been diagnosed with genital herpes, call your doctor if you are having frequent outbreaks or if you can't pass urine or are constipated.
If you are pregnant and have genital herpes, or if you think you have genital herpes, tell your doctor.
Watchful waiting
Watchful waiting is a wait-and-see approach. If you have only occasional outbreaks of genital herpes and are comfortable with home treatment, watchful waiting may be all you need.
Exams and Tests
Your doctor may be able to diagnose genital herpes by examining you, especially if the sores look like herpes. If this is your first outbreak, your doctor may take a sample of fluid from the sore for testing. Testing can help the doctor be sure that you have herpes. You may also have a blood test.
Your doctor may ask about your symptoms. For example, you may be asked if you:
- Have sores in your genital area.
- Have any discharge from your vagina or penis.
- Urinate often, or if it burns or stings when you urinate.
The doctor may ask you questions about your risk factors. These are things that make you more likely to get an infection. For example, the doctor may ask about your sexual practices. You may be asked if you use condoms.
Learn more
Treatment Overview
Although there's no cure for genital herpes, treatment can help.
Treatment includes:
- Medicines. Antiviral medicines are the recommended treatment. They can be taken during an outbreak to relieve pain and discomfort and help sores heal faster. They work best if you start them as soon as possible after an outbreak begins. If you have a lot of outbreaks, medicines can also be taken every day. This helps reduce spreading the virus to others and helps limit the number of outbreaks.
- Home treatment. Examples include taking warm sitz baths and wearing cotton underwear. These may help relieve discomfort from sores.
Finding out that you have herpes may cause you to feel a range of emotions. Talking to your partner, a counselor, or a support group may help.
Self-Care
- Be safe with medicines. Take your medicines exactly as directed. Call your doctor if you think you're having a problem with your medicine. You'll get more details on the specific medicines your doctor prescribes.
- To reduce the pain and itching from herpes sores:
- Take warm sitz baths.
- Keep the sores clean and dry in between baths or showers. You can let the sores air-dry. This may feel better than using a towel.
- Wear cotton underwear. Cotton absorbs moisture well.
- Try pouring warm water over the area while urinating. This can help prevent urine from irritating the sores.
- Take an over-the-counter pain medicine, such as acetaminophen (Tylenol), ibuprofen (Advil, Motrin), or naproxen (Aleve). Read and follow all instructions on the label. Do not take two or more pain medicines at the same time unless the doctor told you to. Many pain medicines have acetaminophen, which is Tylenol. Too much acetaminophen (Tylenol) can be harmful.
- Reduce or avoid things that trigger outbreaks for you. These may include fatigue, stress, overexposure to sun, and irritation of the genital area. This can help lower the risk of repeated outbreaks.
Learn more
Related Information
Credits
Current as of: May 5, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: May 5, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.